How AI Automates Insurance Verification for Healthcare Providers
AI is transforming insurance verification in healthcare by automating eligibility checks, reducing manual errors, and speeding up workflows. Instead of relying on calls and portals, AI systems verify coverage in real time, improving claim accuracy and patient experience. For healthcare providers, this means fewer denials, faster payments, and more efficient operations, making AI-powered verification a key part of modern healthcare automation.

Table of Contents
If you have ever worked with a hospital billing team, you already know this: insurance verification is slow, messy, and honestly a bit frustrating. Front desk staff spend hours calling payers, switching between portals, checking eligibility, and still claims get denied. Patients wait longer. Revenue gets stuck. And everyone is tired of repeating the same steps every single day.
The strange part is that everyone knows this process is inefficient, but it still happens. Most of the work is repetitive, structured, and rule-based, which means a lot of it does not actually need constant human effort. That is exactly where AI starts to make sense.
AI can automate insurance verification end to end. Not just partially and not just as a small assistant layer. It can handle eligibility checks, validate details, flag issues, and push verified data into downstream systems in minutes instead of hours.
In this guide, we will look at how AI automates insurance verification, where it fits into healthcare workflows, and what it practically means for providers trying to reduce denials and speed up operations.
What Is Insurance Verification in Healthcare?

Insurance verification is the process of confirming whether a patient’s insurance is valid and what exactly it covers before care is delivered. On the surface, it sounds simple. In practice, it is often more complicated than it should be.
A proper verification process usually checks:
Patient eligibility
Active coverage status
Co-pay and deductible details
Policy limitations
Pre-authorization requirements
Coverage for specific procedures or services
Ideally, this happens before treatment begins. But in many organizations, verification is rushed, delayed, or incomplete. When that happens, claim denials show up later, and fixing them takes far more time than verifying things properly in the first place.
That is why insurance verification matters so much. It may look like a small administrative task, but it directly affects billing accuracy, patient satisfaction, and overall cash flow.
Challenges of Manual Insurance Verification
Manual verification is still common across healthcare, but it creates the same problems again and again.
It consumes too much time
Staff often spend hours calling insurance companies or logging into multiple payer portals. In many cases, they wait on hold longer than the actual verification takes.
Errors happen frequently
Even experienced teams can miss details such as outdated coverage information, incorrect codes, or incomplete policy data. Small mistakes at this stage often become major billing issues later.
Staff burnout builds over time
Repeating the same verification process every day is tedious work. It slows teams down, increases frustration, and reduces morale in roles that are already under pressure.
Delays in patient onboarding
Patients are sometimes asked to wait because verification is not complete. In some cases, appointments or treatments are delayed simply because the back-office process is still catching up.
Revenue leakage increases
Denied claims, manual rework, and missed coverage details all affect collections. You may not feel the impact immediately every day, but over time it becomes very visible in the revenue cycle.
Lack of real-time updates
Insurance data changes quickly. Manual processes often depend on outdated information or one-time checks that do not reflect real-time payer updates.
What Is AI-Powered Insurance Verification?
AI-powered insurance verification uses intelligent systems to automate eligibility and coverage checks with little or no manual intervention. Instead of people repeating structured tasks across calls, portals, and spreadsheets, AI handles those steps automatically.
A typical AI-based verification system can:
Extract patient data from forms or uploaded documents
Validate and standardize information
Connect with payer systems in real time
Verify eligibility and coverage details
Flag missing, incorrect, or inconsistent data
Some platforms use natural language processing to read insurance documents and payer responses. Others connect directly to payer systems and clearinghouses through APIs. The goal is not to replace staff completely. It is to remove repetitive work so teams can focus on exceptions, patient support, and higher-value decisions.
How AI Automates Insurance Verification Step by Step
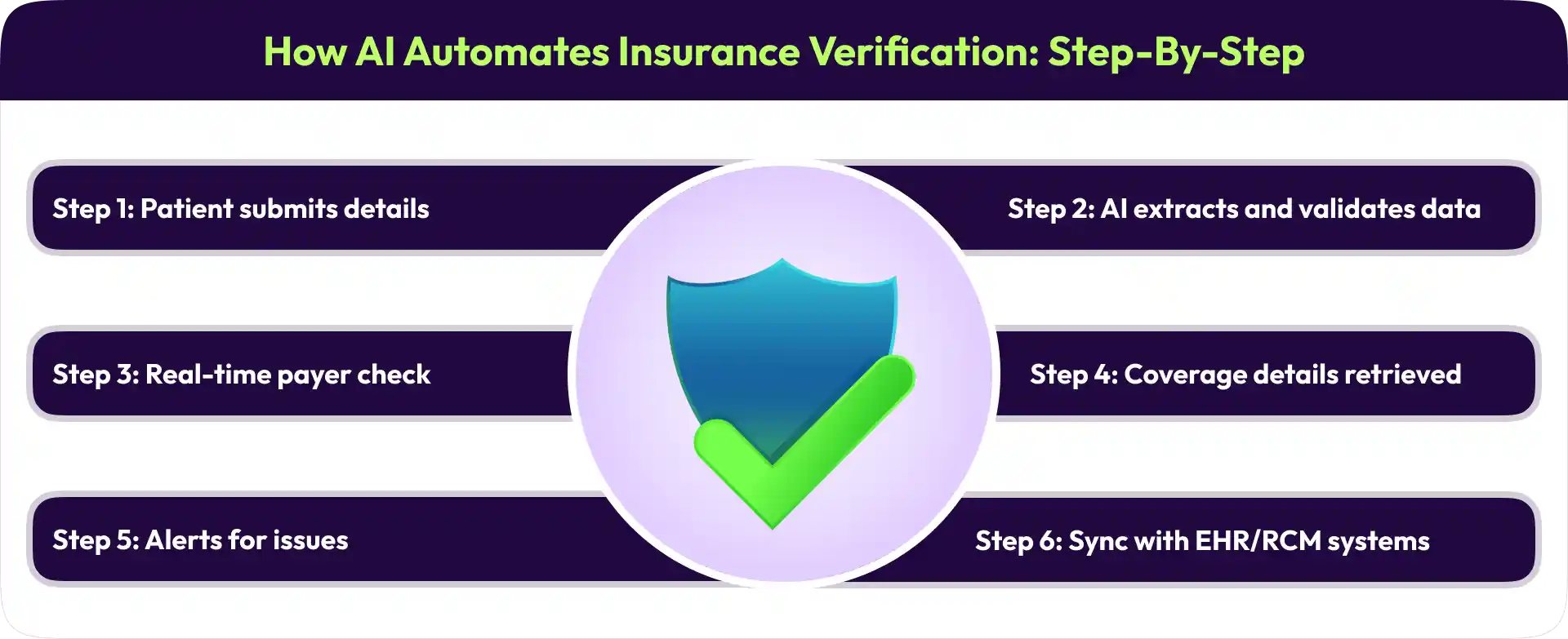
A real-world AI verification workflow usually looks something like this.
Step 1: Patient details are submitted
The patient shares insurance information online, through a mobile app, or at the front desk during intake.
Step 2: AI extracts and validates the data
AI reads the submitted information, standardizes formats, checks for missing fields, and identifies obvious issues early. For example, if a policy number is incomplete or the subscriber name does not match, the system can flag it immediately.
Step 3: Real-time payer verification begins
The system connects with payer databases, clearinghouses, or integrated verification services to confirm eligibility in real time. This removes the need for manual calls, hold times, and repeated portal logins.
Step 4: Coverage details are retrieved
AI pulls the most important information needed for billing and intake, including co-pays, deductibles, service eligibility, policy limits, and pre-authorization requirements.
Step 5: Issues are flagged automatically
If something looks wrong, such as an expired policy, data mismatch, or missing requirement, the system alerts staff right away so the issue can be resolved before treatment or claim submission.
Step 6: Verified data syncs with internal systems
Once verification is complete, the information can be pushed into EHR, practice management, billing, or revenue cycle systems automatically. That eliminates duplicate data entry and keeps downstream workflows cleaner.
Taken together, this removes most of the friction that slows insurance verification down today.
Still verifying insurance manually? It takes time, leads to small mistakes, and slows everything down. With AI, insurance verification can happen in minutes without constant calls, back and forth, or extra workload on your team. If you want to see how this could fit into your current setup, our team can walk you through it.
Key Benefits of AI in Insurance Verification
This is where providers start seeing practical value.
Faster verification
Eligibility checks happen in minutes instead of hours, and in some cases almost instantly.
Fewer claim denials
More accurate insurance data reduces avoidable errors at the very beginning of the revenue cycle.
Better patient experience
Patients spend less time waiting for confirmation and are less likely to face billing confusion later.
Lower operational costs
Reducing repetitive manual work means teams can handle more volume without expanding administrative overhead at the same pace.
Scalable workflows
As patient volume grows, AI can manage larger verification loads without creating the same level of operational slowdown.
Improved compliance and auditability
AI systems can maintain logs automatically, which helps organizations track verification activity more consistently.
More predictable billing operations
When verification is consistent, claims creation and billing workflows become more stable and easier to manage.
Real-World Use Cases of AI Insurance Verification
AI-powered insurance verification works across different healthcare environments, though the exact workflow can vary based on volume, complexity, and care model.
Hospitals and multi-specialty clinics
Large hospitals handle hundreds or thousands of verifications each day. Manual processes do not scale well in that environment. AI helps verify insurance in bulk and in real time, reducing front-desk bottlenecks and improving data quality before billing teams get involved.
Telehealth platforms
Telehealth depends on fast onboarding. AI can verify coverage during the appointment booking process itself, so eligibility is confirmed before the consultation starts.
Diagnostic labs
Labs often run into problems when tests are completed before coverage is fully verified. AI helps verify eligibility upfront, reducing billing disputes and making expectations clearer for patients.
Specialty care providers
In specialties such as oncology, cardiology, or orthopedics, verification is often more complex because procedure coverage and pre-authorization requirements matter. AI helps teams check those requirements more consistently and surface exceptions earlier.
How AI Verification Supports Revenue Cycle Management
Insurance verification sits right at the start of the revenue cycle. If it goes wrong there, the problems flow downstream into claims, denials, collections, and reimbursement timing. This is where AI starts creating financial impact, not just operational convenience.
Cleaner claims from the beginning
When insurance data is verified accurately upfront, claims are less likely to be rejected for basic errors. That reduces rework later.
Improved first-pass claim acceptance
Claims that are verified properly before submission have a better chance of being accepted the first time, which means fewer corrections and fewer delays.
Faster reimbursements
When claims do not get caught in preventable denial loops, payments move faster and cash flow becomes easier to manage.
Reduced administrative overhead
Manual verification demands a lot of staff time. AI reduces that load so providers can scale operations without relying entirely on adding more headcount.
Better financial visibility
Over time, AI systems can show verification outcomes, denial patterns, payer behavior, and recurring coverage gaps. That visibility supports better operational decisions.
Integration with Existing Healthcare Systems
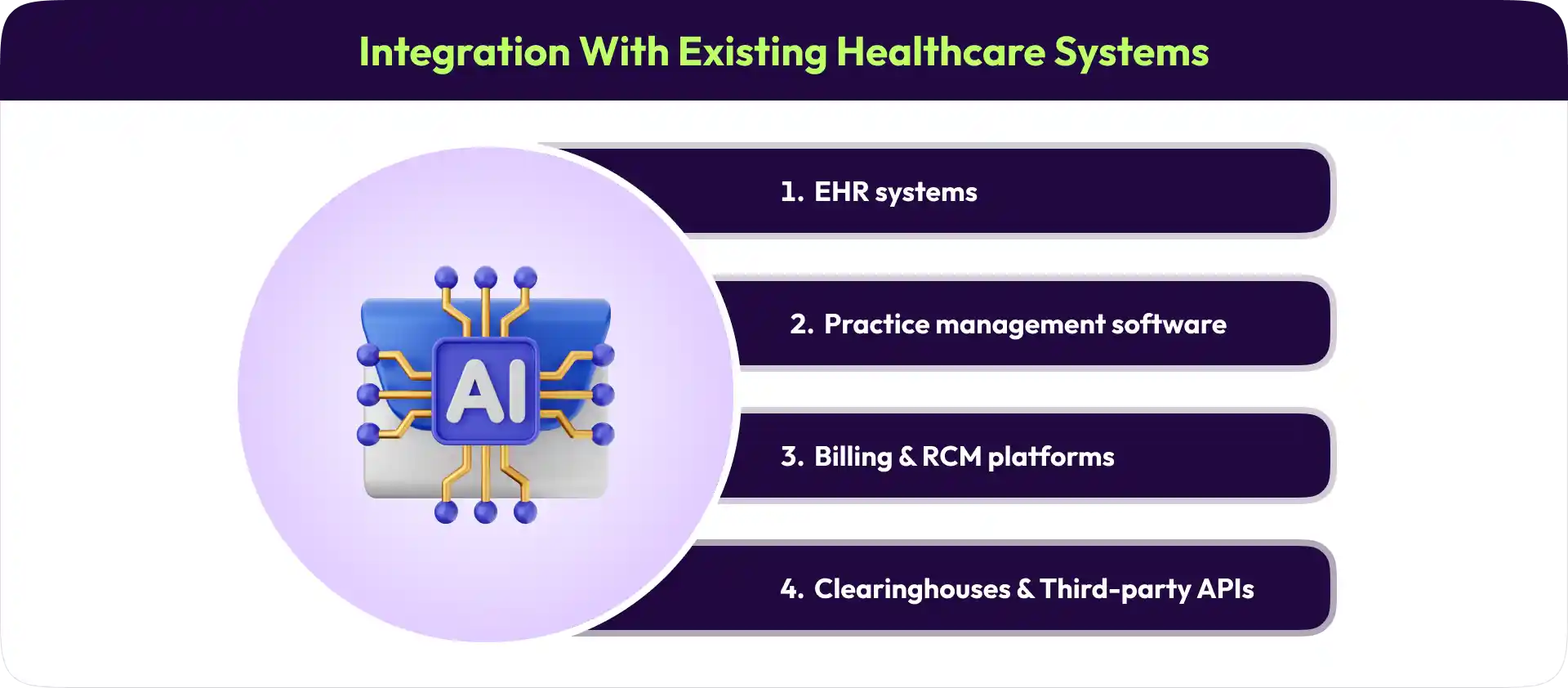
One of the biggest concerns providers have is whether AI will disrupt existing workflows or require replacing core systems. In most cases, that is not how these solutions are implemented. They are usually designed to integrate with the tools providers already use.
EHR systems: Verified insurance data can be pushed directly into patient records, reducing manual entry.
Practice management software: Scheduling, intake, and verification can work together without creating extra steps.
Billing and RCM platforms: Verified information can flow into claims and billing systems automatically.
Clearinghouses and payer systems: Many AI tools connect directly for faster real-time eligibility checks.
Third-party APIs: AI can often sit quietly in the background while existing workflows continue largely unchanged.
That said, integration is not always instant. Legacy environments and highly customized systems may take more effort, but in most cases the challenge is manageable with the right implementation approach.
Challenges and Considerations
AI is useful here, but it is not perfect. Providers should think through the practical considerations before rolling it out.
Data privacy and compliance
Healthcare data is sensitive, so any verification solution must align with HIPAA requirements and internal security standards.
Integration complexity
If the current environment is outdated or heavily customized, implementation can take longer than expected.
Initial investment
There is usually an upfront cost in software, setup time, and internal coordination. The return can be strong, but the first step still requires commitment.
Staff adaptation
Even when the technology works well, teams need time to adjust. Change management matters just as much as the tool itself.
Dependence on input quality
AI improves accuracy, but it still depends on the quality of the data it receives. Incomplete or inconsistent patient information can still affect outcomes.
The Future of AI in Insurance Verification
The direction here is becoming pretty clear. Insurance verification is moving toward faster, more connected, and more intelligent workflows.
Real-time verification ecosystems: Providers and payers are moving toward faster connected systems where coverage checks happen almost instantly.
Predictive verification: AI will increasingly identify likely denial risks before the claim is even submitted.
AI agents for end-to-end workflows: Verification will connect more deeply with intake, billing follow-ups, and downstream revenue cycle tasks.
More complete RCM automation: Verification is likely to become one of the foundational layers of broader revenue cycle automation.
This will not happen all at once, but the shift is already visible.
How to Choose the Right AI Insurance Verification Solution
Not every AI platform performs well outside a demo environment, so choosing the right solution matters more than many teams expect.
Look for a solution that offers:
Accurate verification results
Smooth integration with your current systems
Strong security and compliance controls
Workflow customization based on your operational needs
Reliable support and onboarding
Where Alris AI fits in
This is where platforms like Alris AI become relevant. Instead of automating only one isolated step, Alris focuses on connected workflow automation across operations.
Automate insurance verification
Handle follow-ups through email or SMS
Answer questions using internal documents and operational knowledge
Trigger actions across connected systems
So the value is not just faster verification. It is better workflow continuity across the full process. The right next step is to see how that fits into your current setup, because every organization is a little different.
Conclusion
Insurance verification has always been one of those tasks that seems small but ends up affecting everything. When it is handled manually, it slows teams down, creates avoidable errors, and contributes to claim denials that could have been prevented.
AI does not change the whole system overnight, but it does improve one of the most repetitive and error-prone parts of the workflow. It makes verification faster, more consistent, and easier to manage without increasing the burden on your staff.
Adoption still takes planning. Integration, cost, and team adjustment all matter. But once the system is in place, the operational difference becomes noticeable quickly.
If your team is still spending hours verifying insurance or dealing with repeated denials tied to eligibility issues, it may be time to rethink the process. Not every workflow needs automation, but this one usually does.
If insurance verification is slowing your team down, it is not just a process issue. It is a revenue issue. Manual checks, delays, and repeated errors quietly affect cash flow. AI can improve this, but only when it fits into your existing workflow without adding more complexity. We help healthcare providers simplify verification using AI step by step.
Frequently Asked Questions (FAQs)
1. What is AI insurance verification in healthcare?
AI insurance verification is a system that automatically checks patient insurance details such as eligibility, active coverage, and benefits in real time. It reduces manual calls and helps providers verify coverage faster.
2. How does AI verify patient insurance automatically?
AI collects patient information, validates it, connects with payer systems or clearinghouses, and checks eligibility, benefits, and coverage details automatically. It can also flag missing or incorrect information before claims are submitted.
3. Can AI reduce claim denials in healthcare?
Yes. AI helps reduce preventable denials by verifying insurance details more accurately before services are billed or claims are submitted.
4. How accurate is AI insurance verification?
AI verification is typically more consistent than fully manual processes because it follows defined checks, reduces repetitive human error, and can work with real-time payer data.
5. Is AI insurance verification HIPAA compliant and secure?
Most enterprise-grade healthcare AI solutions are designed to support HIPAA compliance and strong data security standards, but providers should still evaluate each vendor’s safeguards carefully.
6. Can AI integrate with EHR and billing systems?
Yes. Many AI verification tools integrate with EHR, practice management, billing, and revenue cycle systems so verified data can flow automatically across workflows.
7. How can healthcare providers get started with AI insurance verification?
A good first step is to review your current verification workflow, identify where delays or denials occur, and choose a solution that fits your systems and team. Platforms like Alris AI can help automate verification while connecting related operational tasks.
Share This Article
If you found this article helpful, share it with your network

Shravan Rajpurohit
CEO & Co-Founder
Shravan Rajpurohit is the Co-Founder & CEO of The Intellify, a leading Custom Software Development company that empowers startups, product development teams, and Fortune 500 companies. With over 10 years of experience in marketing, sales, and customer success, Shravan has been driving digital innovation since 2018, leading a team of 50+ creative professionals. His mission is to bridge the gap between business ideas and reality through advanced tech solutions, aiming to make The Intellify a global leader. He focuses on delivering excellence, solving real-world problems, and pushing the limits of digital transformation.
Stay Updated with AI Insights
Get the latest articles on AI, automation, and enterprise technology delivered to your inbox weekly.
No spam. Unsubscribe anytime.
Ready to Transform Your Workflows?
Join thousands of businesses already using Alris to automate their operations and boost productivity.


