Insurance Claims Automation: How AI Transforms Claims Processing End-to-End

Insurance claims are where everything gets tested. A customer does not really care how good a policy sounds until they actually file a claim. And if that process feels slow, unclear, or repetitive, frustration shows up almost immediately.
That is exactly why insurance claims automation is becoming so important. It is not just about saving time internally. It is about delivering a smoother and faster experience when policyholders need support the most. Let us break it down step by step.
What Is Insurance Claims Automation?
In simple terms, insurance claims automation means using technology to handle repetitive and time-consuming tasks across the claims process. Earlier, most of this work was handled manually.
A customer would report a claim, someone would note it down, another team would verify the details, emails would move back and forth, and documents would be reviewed manually. It worked, but it was far from efficient.
Now, automation changes that, but there is an important difference worth understanding.
Basic automation follows fixed rules
AI-driven automation understands context, learns from patterns, and takes action
With AI in insurance claims, systems do not just follow instructions. They can read documents, extract important details, make decisions within defined rules, and trigger the next steps automatically.
Insurers are moving in this direction because customer expectations have changed. People do not want to wait days for updates anymore.
How Insurance Claims Processing Works
At a high level, a typical insurance claims process usually follows a sequence like this:
Claim is reported
A customer reaches out through a call, app, email, or website. In many cases, this first interaction shapes how smooth the process feels overall.
Details are captured
Information such as policy number, incident type, date, and location is recorded. If this step is incomplete or inconsistent, it often creates problems later.
Documents are submitted
Customers send or upload required documents. Depending on the claim, this could include hospital bills, repair estimates, incident reports, or accident photos. This stage often involves repeated follow-ups.
Claim is reviewed
The insurer checks whether the claim is valid under the policy coverage. Teams review documents, verify the facts, and cross-check information across systems.
Decision is made
Based on the evaluation, the claim is approved, rejected, or returned for clarification.
Payment is processed
Once approved, the payout is initiated. Even here, additional checks and internal coordination can add delays.
Customer is informed
Updates are shared through calls, email, or SMS, though not always in real time.
On paper it looks straightforward, but each step can slow down when too much of the process depends on manual work.
Where the Traditional Claims Process Slows Down
This is where most insurers start to feel the pressure. Traditional claims workflows often break down in the same places.
Manual data entry across systems
The same claim details are often entered into multiple tools. That repetition wastes time and increases the chance of errors.
Communication delays
Claims teams still rely heavily on calls and email. If one response is delayed, the entire process starts slowing down.
Incomplete documentation
Customers often miss required files or submit incorrect information. That creates more back-and-forth and increases the claim cycle time.
Approval bottlenecks
Claims sit in queues waiting for review. During high-volume periods, these backlogs can grow fast.
Lack of visibility
Customers do not always receive real-time updates, so they end up calling support for status checks, which adds even more load on internal teams.
Dependence on manual coordination
Different teams manage different stages of the claim, and handoffs are not always smooth. That creates a constant cycle of follow-ups and delays.
The result is frustration on both sides. Customers feel uncertain, and internal teams end up stuck in repetitive coordination work.
How AI Improves Insurance Claims Automation
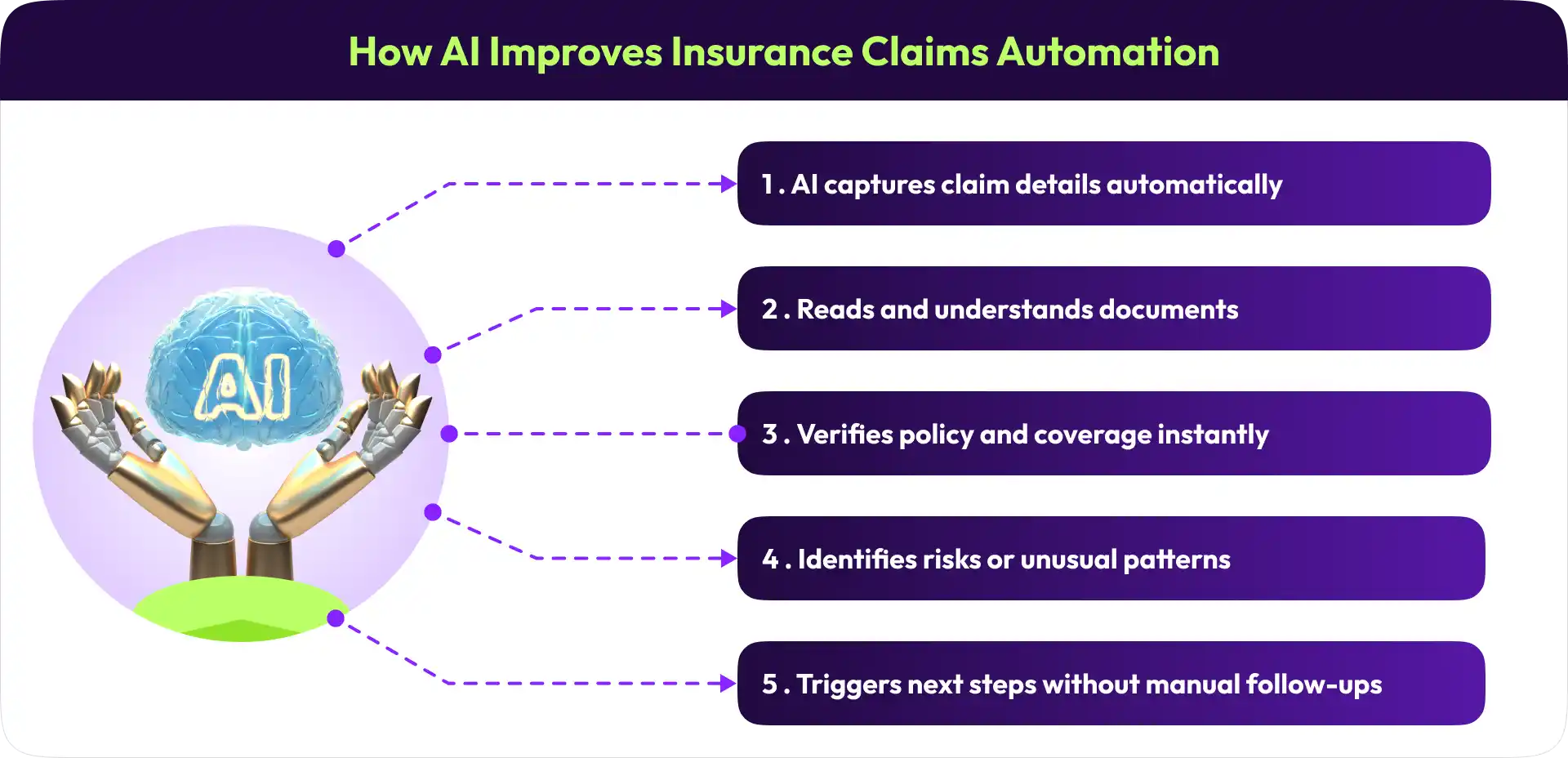
This is where AI starts making a visible difference. Instead of depending on people for every structured step, AI takes ownership of repetitive tasks that used to demand constant manual effort.
Captures claim details automatically from forms, emails, chats, and conversations
Understands documents like bills, reports, and images without manual review
Verifies policy details instantly by connecting with internal systems
Identifies patterns that may indicate risks, mismatches, or inconsistencies
Triggers actions automatically, such as requesting documents or moving the claim forward
What matters most is that AI does not just assist individual tasks. It reduces the need for manual intervention across the workflow, so the system manages routine progress, and teams step in mainly for exceptions and judgment-based decisions.
Step-by-Step: How AI Automates the Claims Process
Claim intake
AI handles incoming claim requests across multiple channels. Whether the customer reaches out through a call, email, or chat, the system understands the request, captures structured data, and ensures all required details are collected. That reduces errors at the very first step.
Data extraction and verification
AI extracts key information from uploaded documents, forms, and images, then verifies it against policy data and internal records. Manual validation work drops sharply here.
Document handling
This is often one of the most time-consuming parts of claims processing, and AI simplifies it by identifying missing documents, sending reminders automatically, and organizing files in a structured way. Teams do not have to keep chasing paperwork.
Claim assessment
AI evaluates claims using predefined rules and available data. It checks eligibility, identifies mismatches, and flags more complex cases. Straightforward claims can move ahead quickly, while unusual ones are escalated for review.
Decision and approval
For simple claims, AI can apply decision rules and route the case toward approval. For exceptions, it sends the claim to the right team with the relevant context already attached, which speeds up decision-making.
Settlement and communication
Once a claim is approved, payment workflows can be triggered automatically, and customers can receive instant status updates. This improves transparency and reduces uncertainty throughout the settlement phase.
Manual vs AI-Driven Claims Processing: What Changes
The difference is not just operational. It becomes visible at every stage of the claims journey.
Speed
Manual claims processing often creates delays at every stage. AI helps move claims faster from one step to the next.
Effort
Manual workflows depend heavily on people coordinating repetitive tasks. AI reduces that workload and lets teams focus on higher-value work.
Accuracy
Manual processing is more prone to inconsistency and missed details. AI supports more structured and repeatable data handling.
Customer experience
Traditional workflows often give customers limited visibility and slow updates. AI enables faster communication and more real-time progress tracking.
Scalability
Manual operations struggle when claim volumes spike. AI-driven workflows can handle many claims at once without creating the same level of operational strain.
Real Use Cases of AI in Insurance Claims
AI-powered claims automation is already useful across multiple insurance lines.
Auto insurance
AI can analyze accident details, process claims faster, and even support damage assessment using uploaded images.
Health insurance
Health insurers deal with large volumes of medical bills, treatment records, and supporting documents. AI helps organize, extract, and validate this information faster.
Property insurance
Property claims often require damage assessment, documentation review, and faster handling during peak claim events. Automation helps accelerate these workflows.
Travel insurance
Claims related to delays, cancellations, or lost baggage can be processed much faster when intake, validation, and communication are automated.
Microinsurance and small claims
For low-value and rule-based claims, AI can support near-instant decisions and approvals, improving customer satisfaction while reducing manual review effort.
These examples show that claims automation is not limited to one insurance segment. It applies wherever insurers handle repetitive claim workflows at scale.
Key Benefits of Insurance Claims Automation
When implemented well, insurance claims automation delivers measurable improvements across operations and customer experience.
Faster processing times: Claims move more quickly from intake to settlement
Reduced manual workload: Teams spend less time on repetitive tasks
Improved accuracy: Fewer errors in data handling and validation
Better customer experience: Faster updates and less waiting
Lower operational costs: Reduced dependency on manual effort
Improved team efficiency: Employees focus on complex and high-value tasks
Over time, these gains compound and improve the overall performance of the claims function.
What to Consider Before Automating Claims
Before implementing claims automation, insurers should think through a few practical areas.
Integration with existing systems: Your CRM, policy systems, and claims tools should connect smoothly
Data quality: If your data is inconsistent, automation won’t work effectively
Compliance requirements: Insurance processes must meet regulatory standards
Human oversight: Not every decision should be automated, some cases need judgment
Change management: Teams need to adapt to new workflows
Choosing the right use case: Start with processes that deliver quick value
A structured rollout reduces risk and gives insurers a better chance of achieving measurable outcomes early.
How to Get Started with Insurance Claims Automation

Getting started with insurance claims automation may sound like a big shift, but it does not have to be overwhelming. The key is to improve one part of the process at a time rather than trying to transform everything at once.
1. Identify repetitive and time-consuming tasks
Start by looking at where teams spend the most time. Data entry, document follow-ups, and status updates are usually strong candidates for early automation.
2. Map the current workflow clearly
Document each step from claim intake to settlement. This makes it easier to spot delays, repeated handoffs, and unnecessary friction.
3. Pick one area to start (don’t do everything at once)
Pick a focused area such as claim intake, document collection, or status communication. Starting small makes testing and refinement easier.
4. Choose tools that fit existing systems
Automation works best when it connects with your current CRM, policy systems, and claims tools instead of forcing a full replacement.
5. Set clear goals and track results
Define measurable outcomes such as faster processing time, fewer errors, or reduced manual workload, then track those metrics from the start.
6. Involve the team early
The people using the workflow every day should be part of the rollout. Their feedback improves adoption and reveals issues faster.
7. Test, refine, and scale gradually
Once the first use case performs well, automation can be extended to other parts of the claims process with less risk and more confidence.
The goal is not to replace the entire system overnight. It is to improve the claims workflow step by step until the overall operation becomes faster and more manageable.
How AI Fits into Real Insurance Claims Workflows
This is where things become practical. Modern AI systems do not just assist teams. They can operate across workflows.
AI agents can handle calls, emails, and claim requests in one place
They capture and process claim data without repeated manual input
They execute actions across systems instead of only suggesting next steps
Workflows continue without constant follow-ups
Teams get relief from repetitive administrative work
Platforms like Alris AI bring communication, data handling, and workflow execution into one connected system. The goal is not to replace teams, but to free them up for the work that genuinely needs human judgment.
The Future of AI in Insurance Claims Processing
Looking ahead, the shift toward automated claims processing will continue to accelerate.
Faster end-to-end processing: Claims will move from reporting to settlement much quicker
More self-service options: Customers will handle claims directly through apps or portals
Better fraud detection: AI will identify patterns that humans might miss
Stronger system integration: Different tools will work more seamlessly together
AI handling complete workflows: Not just assisting, but managing entire processes
It will not all happen overnight, but the direction is clear. Insurers that adapt early will be in a stronger position to improve service quality and operational efficiency at the same time.
Conclusion
Insurance claims automation is no longer just an efficiency upgrade. It is steadily becoming a necessity. As claim volumes rise and customer expectations increase, relying only on manual processes makes it much harder for insurers to keep up.
AI helps simplify what used to feel like a fragmented and time-consuming process. It reduces delays, removes repetitive work, and keeps claims moving without constant follow-ups. For teams, that means less operational pressure. For customers, it means faster answers and fewer uncertainties.
That said, automation does not replace people. It supports them. The goal is to let systems handle routine and high-volume tasks while human teams focus on the decisions that truly require judgment.
When done well, insurance claims automation improves both sides of the experience: internal operations and customer satisfaction. And that balance is exactly what most insurers are trying to achieve now.
Frequently Asked Questions (FAQs)
1. Which parts of the insurance claims process are easiest to automate first?
Claim intake, document collection, and basic verification are usually the easiest places to start. These tasks are repetitive and rule-based, so automation can reduce manual work quickly and improve processing speed without disrupting the full operation.
2. How does AI handle unstructured data like emails, PDFs, and images in claims?
AI can read emails, PDFs, and images, extract the important details, and convert that information into structured data. This reduces manual entry and helps claims move through the workflow faster and with better consistency.
3. How do insurers decide which claims can be fully automated?
Insurers typically automate simple and low-risk claims using predefined rules. AI analyzes the claim data and flags complex, unclear, or higher-risk cases for human review so control and accuracy are maintained.
4. Can insurance claims automation work with existing systems, or does it require replacement?
In most cases, claims automation works by integrating with existing systems. It connects data and workflows across tools, which helps insurers improve claims processing without replacing their entire core platform.
5. Does claims automation reduce the need for human involvement completely?
No. Automation handles repetitive and structured work, but people are still essential for exceptions, complex cases, escalations, and final decisions where judgment matters.
6. How long does it take to implement insurance claims automation?
It depends on the scope. Focused automation use cases can often be implemented within a few months, while broader claims transformation programs are usually rolled out in phases over a longer period.

Shravan Rajpurohit
CEO & Co-Founder
Shravan Rajpurohit is the Co-Founder & CEO of The Intellify, a leading Custom Software Development company that empowers startups, product development teams, and Fortune 500 companies. With over 10 years of experience in marketing, sales, and customer success, Shravan has been driving digital innovation since 2018, leading a team of 50+ creative professionals. His mission is to bridge the gap between business ideas and reality through advanced tech solutions, aiming to make The Intellify a global leader. He focuses on delivering excellence, solving real-world problems, and pushing the limits of digital transformation.

Stay Updated
with AI Insights
Get the latest articles on AI, automation, and enterprise technology delivered to your inbox weekly.
500+ people have already subsribed!
No spam. Unsubscribe anytime.


